Both laser therapy and shockwave therapy are commonly used modalities for pain relief and tissue healing in multiple musculoskeletal (MSK) pathologies. In this blog, we will explore these two modalities, their physiological effects, similarities, and differences, with respect to MSK pathologies.
Laser Therapy
Laser therapy is a non-invasive treatment option that uses light energy to penetrate tissue and promote healing. Low-level laser therapy, also known as cold laser
therapy, is a non-invasive treatment that uses specific wavelengths of light to penetrate tissue and stimulate cell growth and repair. The physiological effects of
laser include reductions in pain, blood flow, oedema, inflammation, muscle spasm, and metabolic demand (Malanga & Stark, 2015).
There are two classes of lasers commonly used by therapists; class 3 and 4. Class 3 lasers are less than 500 milliwatts (mw) in power while class 4 lasers are greater than 500 mw. Class 3 lasers are sometimes referred to as cold lasers, and the therapy may be called LLLT for low-level laser therapy. In contrast, class 4 laser therapy is sometimes called HPLT for high-power laser therapy.
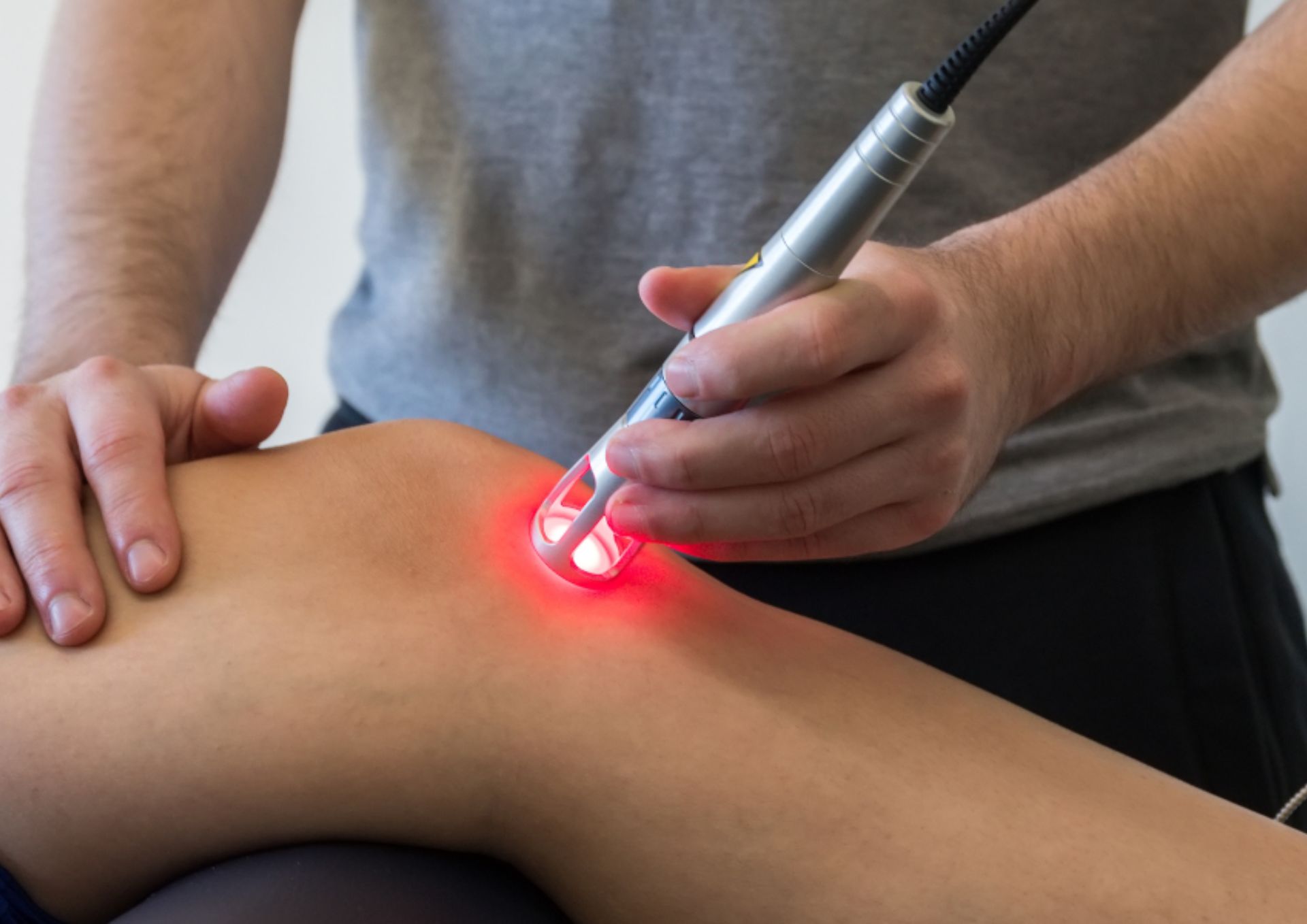
It is a non-invasive, painless treatment option that can be used alone or in combination with other therapies. Overall, laser therapy has shown promise in the treatment of musculoskeletal pathologies, but further research is needed to fully understand its effectiveness and optimal application.
Laser depth of penetration
Due to their extremely low power output, these “Cold Lasers” are incapable of targeting deeper tissues. Most laser radiations are absorbed within the first 1mm of skin. Mathematical simulations and data from the literature suggest that the depth of penetration of laser radiation using wavelengths from 630nm up to 1100 nm, can be up to 50mm (Esnouf et al, 2007).
Shockwave Therapy
Shockwave therapy is a non-invasive treatment that uses acoustic waves to transmit sound waves to tissues for therapeutic benefits. This therapy has been found to be
beneficial in treating various musculoskeletal pathologies such as tendinopathy in areas such as the rotator cuff, lateral and medial epicondyles, greater trochanter,
proximal hamstring origin, Achilles, and plantar fascia. Shockwave therapy is beneficial in decreasing pain and increasing functionality by triggering the body’s healing process (Chung & Wiley, 2002). It can also increase circulation around injured soft tissues, break down calcified deposits, and stimulate cells that generate new bone tissue (Kieves et al, 2015).
Shockwave depth of penetration
The depth of penetration of shockwave therapy can vary depending on the type of shockwaves used. Radial shockwave therapy employs a ballistically generated pressure wave that radiates out from the applicator’s surface, providing a depth of penetration of 3-5 cm, which can vary based on the transmitter used. It is typically used to address superficial soft tissue conditions, such as tendinopathies, plantar fasciitis, and trigger points. In contrast, focused shockwave therapy concentrates the shockwave energy into a more specific area using an electromagnetic coil. This technique allows for greater depth penetration, up to 6-12 cm, making it ideal for treating deeper soft tissue conditions such as non-union fractures, avascular necrosis, and chronic tendinopathies.

Key differences between the two modalities
Both laser therapy and shockwave therapy are used for treating soft tissue injuries and to decrease inflammation and pain to facilitate the healing process. However, there are some key differences between the two modalities:
Photonic energy delivery: Laser therapy imparts photonic energy into tissue to create photochemical changes at the mitochondrial level through photo-biomodulation (PBM), whereas therapeutic shockwave devices deliver high- energy sound waves into tissues.
Depth of Tissue: Shockwave is capable of targeting both superficial and deeper structures, whereas laser therapy’s effectiveness is limited to superficial structures.
Calcific tendonitis, also known as calcific tendinopathy, is a common cause of tendon pain that can affect various areas of the body, with the shoulder being the most frequently affected site, followed by the hip. Patients with calcific tendonitis who undergo shockwave therapy often experience a reduction in pain and improved function due to the break-up of the calcific deposits and promote faster healing.
Compatibility: While both laser and shockwave therapies have similar applications and exert similar properties on their target tissues, they are considered separate and yet compatible and complementary therapies.
Advantages of Shockwave therapy versus laser therapy
Shockwave therapy is a highly effective option for treating chronic tendinopathy, offering several advantages over laser therapy. Unlike laser therapy, shockwave
therapy can have a deeper and stronger effect and also break down calcified deposits, making it a more comprehensive solution for a wider range of conditions, especially stubborn conditions like insertional Achilles and proximal hamstrings tendinopathy.
While both laser therapy and shockwave therapy are non-invasive, drug-free, and have the potential to relieve pain and improve functionality and quality of life,
shockwave therapy offers a unique approach to treating tendinopathy, especially in chronic and stubborn cases.
If you are interested in learning more about the practical application of SWT, visit our training page with multiple courses on all key areas of MSK practice.
Benoy Mathew, MSc, MCSP
Advanced Practice Physio
MSK SWT Specialist
References:
Chung, B. and Preston Wiley, J., 2002. Extracorporeal shockwave therapy: a review. Sports medicine, 32, pp.851- 865.
Esnouf, A., Wright, P.A., Moore, J.C. and Ahmed, S., 2007. Depth of penetration of an 850nm wavelength low level laser in human skin. Acupuncture & electro-therapeutics research, 32(1-2), pp.81-86.
Kieves, N.R., MacKay, C.S., Adducci, K., Rao, S., Goh, C., Palmer, R.H. and Duerr, F.M., 2015. High energy focused shock wave therapy accelerates bone healing. Veterinary and Comparative Orthopaedics and Traumatology, 28(06), pp.425-432.
Malanga, G.A., Yan, N. and Stark, J., 2015. Mechanisms and efficacy of heat and cold therapies for musculoskeletal
injury. Postgraduate medicine, 127(1), pp.57-65.




